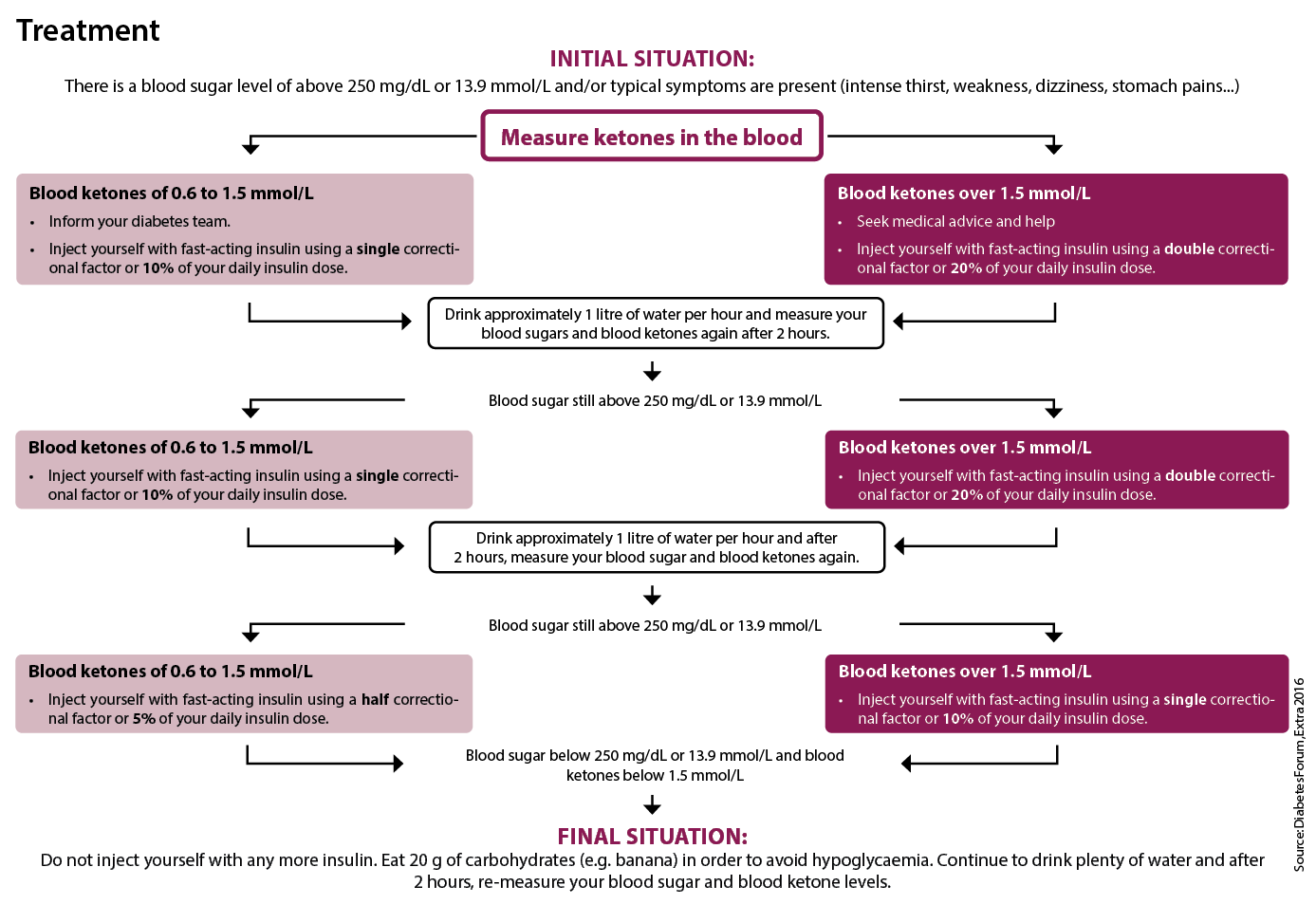
Ketoacidosis - a diabetic emergency
Acidaemia by ketones
Fat is metabolized to produce the necessary energy
For people with diabetes, there are two situations that should be avoided at all costs: severe hypoglycemia and acute blood sugar derailment upwards, which can lead to ketoacidosis. While hypoglycaemia can usually be quickly corrected by the person affected, treatment of ketoacidosis requires more intensive intervention to achieve normal blood sugar levels.
The treatment of ketoacidosis requires good diabetes education with the necessary knowledge. Talk to your doctor about this.
A condition for the development of ketoacidosis is an acute lack of insulin. A person with type 1 diabetes who is completely dependent on insulin injections to regulate his or her carbohydrate metabolism reacts to a sudden insulin deficiency within a few hours with a massive increase in blood sugar levels. This occurs because only insulin can transport the sugar present into the cells to produce energy.
In order to continue to have enough energy available, the body switches to an emergency program. Now fat is metabolized to produce the necessary energy. However, this process produces fatty acids, which cause ketone bodies to form in the liver. This flood of ketones makes our blood acidic. This can develop into a life-threatening process that leads to a change in the pH value of the blood. Normally this value is in a very narrow range (7.35-7.45). Even the smallest deviations from this value disturb normal organ functions, which explains the dangerous nature of this metabolic derailment.
The absolute insulin deficiency that leads to this situation must be treated according to a certain scheme. Without the person's knowledge necessary for treatment, otherwise diabetic ketoacidosis will inevitably lead to emergency treatment in a hospital.
Who is particularly at risk of developing ketoacidosis?
Diabetic ketoacidosis is very often a sign of type 1 diabetes. Many people with diabtes will remember the symptoms during this period. However, even with an existing type 1 diabetes, the risk of ketoacidosis increases when acute and especially febrile diseases and infections occur, because this can cause the insulin requirement to rise dramatically during this period. Since people with type 2 diabetes still have their own insulin reserves, a severe and acute metabolic situation is very rare in this case.
How does ketoacidosis manifest itself?
The first sign in all cases is a highly elevated blood sugar level. If there is no prompt reduction in blood sugar levels, the following symptoms are typical of developing ketoacidosis:
- tiredness, exhaustion or even drowsiness
- excessive urination
- abdominal pain, nausea and even vomiting
- acetone smell in the air we breathe (like nail polish remover or rotten apples)
- enforced breathing
Now it is important to act quickly and with support if possible. A measurement of the blood ketones makes it easier for you to correctly assess the metabolic situation and to monitor the progress of the treatment.
Understanding your blood ketone levels
Ketones are thus formed in the body when fat is used instead of glucose to produce energy because there is not enough insulin. It is a warning sign that your diabetes is out of control or that you are getting sick1.
Your blood sugar is higher than 13.8 mmol/L (250 mg/dL) and your ketone level is2
Lower than 0.6 mmol/L | Normal blood ketone level |
0.6 to 1.5 mmol/L | A moderate ketone level, which may indicate fat metabolism and weight loss, but not insulin deficiency. Measure again at a later time and consult your doctor. |
1.6 to 3.0 mmol/L | A high ketone level with increased risk of diabetic ketoacidosis (DKA). Contact your doctor immediately. |
Higher than 3.0 mmol/L | A serious metabolic condition; immediate emergency treatment is necessary. |
What you can do if your blood ketone level is high or low
The meter displays "HI" or "LO" as the result:
- Treat your diabetes according to your healthcare provider's instructions.
- Check your meter with a control solution, see the "Test with control solution" section.
- Repeat the test with a new test strip. If you get a high or low result again, contact your doctor immediately.
Possibilities of self-control - Determination of blood ketones
For some years now there are blood glucose meters available that can also measure blood ketones with the corresponding ketone test strips. The blood ketone determination is a more accurate, faster (8 seconds) and less conspicuous alternative to the previous urine ketone determination. A beginning ketoacidosis can be detected 1-2 hours earlier in the blood than in the urine. This represents an important window of action for you.
Do causal research to avoid future ketoacidosis!
Even with all caution, ketoacidosis does occur once in a lifetime with diabetes. It is important to take the right action at the right time, to recognise the cause and to act with foresight in order to avoid repeated severe metabolic derailments. Persons who consciously or unconsciously discontinue insulin administration risk insulin supply gaps that lead to massive hyperglycemia within just a few hours. Carriers of insulin pumps should exercise particular caution in this respect. The basal insulin supply must be guaranteed at all times, which means that replacement materials and insulin should always be available. Even during physical activity or a carbohydrate-free meal, the body needs a certain amount of insulin to maintain normal metabolism. Making the right decisions can only be learned through structured training. If necessary, what has been learned should be refreshed.
As a rule, every person concerned knows how he or she should behave in the event of hypoglycaemia, but very few control their blood ketones from an inexplicable blood sugar level of 250 mg/dl (13.9 mmol/l) in order to detect an impending ketoacidosis. Please remember to replace expired ketone test strips in time!
You can find this and other articles as guides for download as PDF.
1. DKA (Ketoacidosis) & Ketones, www.diabetes.org/living-with-diabetes/complications/ketoacidosis-dka html, March 18, 2015
2. Richard M. Weil, Getting to Know Ketones, Diabetes Self –Management 2003 Nov-Dec; 20(6):100-1, 103-4